SENTINEL LYMPH NODE BIOPSY (SLNB)
Sentinel Lymph Node Biopsy Austin
Sentinel Lymph Node Biopsy (SLNB) was originally developed for patients with penile cancer. In an effort to address the limitations of axillary lymph dissection,researchersin the 1980s and 90s adapted this technique for breast cancer patients.
The Sentinel Lymph Node Concept
There are several areas in the body where a group of lymph nodes, known as a lymph node basindrains a relatively specific part of the body. Lymphatic vessels connect lymph nodes in the basin to each other. Examples of lymph node basins are the right and left axillary lymph nodes basins, which drain the breast on the same side.
There is usually onespecific node in a lymph node basinthat is the first node thelymphatic vessels from the area, such as the breast, drain to. The first node in a basin was dubbed the sentinel lymph nodebecause it was thought to act like a soldier or guard whose job is to stand and keep watch.
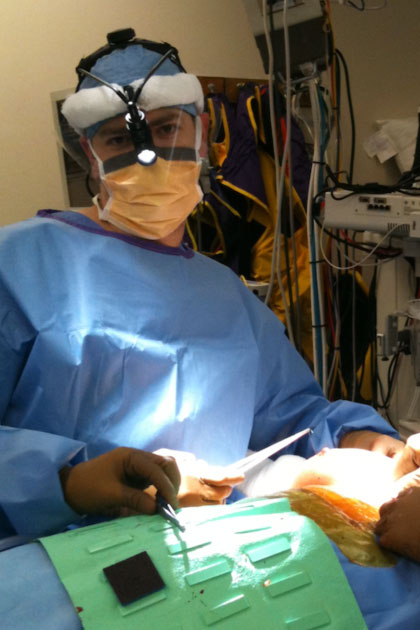
Theoretically, if a cancer cell breaks off the main tumor and travels through a lymphatic vessel system, it will lodge in the sentinel lymph node.Now the sentinel lymph node could kill the cancer cell (yay lymph node) or the cancer cell could multiply (tricky cancer cell). In the case of the multiplying cancer cell, a malignant daughter cell couldbreak away, pass beyond the sentinel node and travel through the lymphatic vessels to other nodes in the basin.
If it were possible to identify the sentinel lymph node and prove it did not contain cancer (negative SLN), one could be pretty certain there wasn’t cancer in the other lymph nodes. Studies show that when done properly, the chance of finding cancer in the other lymph nodes when the SLN is negative is 5% or less. Furthermore, if the sentinel lymph node is negative, an axillary lymph node dissection is not necessary.
Patients with lymph nodes that look normal on physical exam and imaging (clinically node negative) are candidates for sentinel lymph node biopsy (SLNB).
The exception to this is patients with locally advanced cancers and those with inflammatory breast cancer. They are not candidates for SLNB. They should undergo axillary lymph node dissection.
Now a surgeon cannot tell which lymph node in the axilla is the SLN just by looking. In order to identify the SLN, it has to be mapped. There are two ways to map the SLN.
- RadiocolloidThe exact material used varies from institution to institution but basically tiny radioactive beads are attached to lymph cells and suspended in a few drops of salt water. The fluid is injected into the breast. The patient is awake for this. It may sting a little but it is usually well tolerated. Thenthe patient lays on her back with her arm above her head below a large camera suspended above her that detects radioactivity.It will watch as the radioactive material travels through the lymphatic vessels to the sentinel lymph node. Once the camera detects that the radioactive material has been captured by the SLN, the procedure is over. This can take 20 minutes or it can take 2 hours. It just depends on the patient.Sometimes, if surgery is scheduled for first thing in the morning, we do the mapping the day before surgery, usually after 3 PM. Depending on the “half life” or strength of the radioactive material, the lymph node will still be hanging on to it the next morning.Many patients worry they will be radioactive and emit radioactive “stuff” if they go home after injection. Believe me, I’ve had this conversation with several radiation safety officers and been told that the patient “will not be radioactive”,in fact she can “safely hold a baby.”Furthermore, consider this: Thousands of surgeons in this country handle multiple radioactive lymph nodes every day. We hold them, look at them, study them, roll them between our fingers, and measure their radioactivity with a Geiger counter while holding the specimen about 6 inches away from our heart, lungs, thyroid and in some cases, unborn baby. Nurses are in contact with radioactive lymph nodes too as are the folks who carry the specimen from the operating room to the pathology department. Our wonderful pathology colleagues and their personnel are also exposed. Pathologists cut open radioactive lymph nodes for gross evaluation, touch preps, or frozen section.Still skeptical? Rock on. If you can scientifically refute the safety, I invite you to reach out to me. Until then, I trust my colleagues.
- Blue DyeThe sentinel lymph node can also be mapped with blue dye. Original studies used 1% Lymphazurin, also know as Isosulphan Blue. Around 1998, when I began to do sentinel lymph node biopsies, I used Lymphazurin as well andnever had a problem. However, Lymphazurin has been associated with hypersensitivity reactions in a small number of patients.In 2007 there was a nationwide shortage of isosulphan blue so many surgeons switched to methylene blue with the intention of switching back when the time came. However, methylene blue identified the SLN equally as well Lymphazurin and there were no reports of hypersensitive or allergic reactions (as far as I know). So most of us stuck with it.The advantage blue dye has over radiocolloid is that the mapping can be done in the operating room after the patient is asleep. I dilute 2 cc of methylene blue with 2 cc of sterile injectable saline and inject the 4 cc solution into the potential space immediately under the base of the nipple, where the milk ducts emerge from the breast tissue up to the skin of the nipple.Some surgeons inject other places such as over the cancer. Studies have shown that the injection site doesn’t seem to matter. A breast’s SLN is a breast’s SLN. It doesn’t matter how you map it. The SLN is true to its breast. Then the breast is massaged for 5 minutes.
Methylene blue has a few drawbacks:
- Sometimes the skin to turns blue at the site of injection. This is usually temporary but occasionally the blue skin discoloration turns out to be permanent. This should be kept in mind in patients with fair skin who are having breast conservation surgery.
- When injected behind the nipple areolar complex, methylene blue is sometimes associated with nipple necrosis. I would not recommend using it when performing a skin and nipple-sparing mastectomy.
- Methylene blue should NOT be used in pregnant women.
So which technique is better?
The choice of mapping technique depends on the surgeon’s preference and patient circumstances as outlined above. Many times both techniques are used. If the patient has had neoadjuvant chemotherapy, it’s recommended that SLN mapping be done using both radiocolloid and methylene blue and that a minimum of 3 SLNs be removed. Regardless of the mapping technique, the procedure usually takes about one hour. A drain is not placed.
Potential Complications:
- Patients must be aware that in about 5 percent of cases, the SLN cannot be found. When this occurs, a standard axillary lymph node dissection may be necessary.
- Although we refer to sentinel lymph node in the singular, many patients have more than one sentinel lymph node, in fact, the average person has three.
- Sentinel lymph node biopsy is much less likely to result in lymphedema than an axillary lymph node dissection, but it can still happen. All my patients who undergo SLNB are referred to our physical therapists for baseline measurements and are educated on how to detect and prevent lymphedema.
- A relatively common complication of any operation on the axilla is axillary cording. This is when the brachioradialis tendon shortens, causing a “violin string” to appear in the axilla. It can be painful and limit arm range of motion. The good news is that there are physical therapy techniques including message that are very effective at resolving this problem without any permanent sequelae.